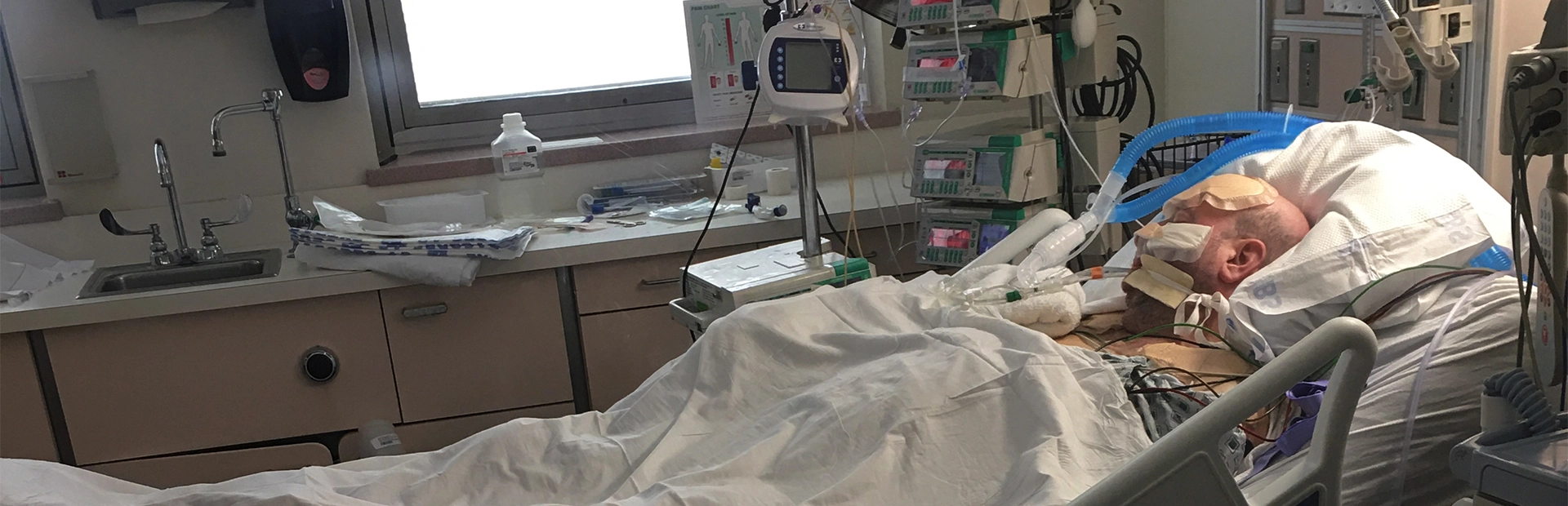
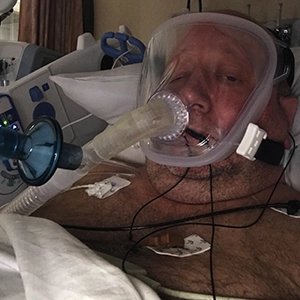
When COVID-19 first arrived in the United States in early 2020, Brian was working at a hospital in Brooklyn. For a month and a half, he worked 12-hour days, seven days a week, making sure that the hospital staff had all the masks, gloves, and other protective equipment they needed. Then, in the first week in April, he began to feel sick and decided to stay home for a day or two. Little did he know that what started as mild cold-like symptoms would end up changing his life. “When I got sick, no one knew what to do. It was at the time when people were going into the hospital and not coming out,” Brian recalled.
His symptoms soon became much more severe, and he rushed to the hospital. At the ER things moved quickly; his oxygen levels dropped rapidly, which meant he had to be hooked up to a CPAP machine. Unfortunately, soon after that, he blacked out and was transferred to a ventilator. He would remain on the ventilator for 38 days, during which time he also required intubation and feeding tubes. Those days were full of constant challenges for his medical team as he went into cardiac arrest three times requiring them to install a temporary pacemaker while he was unconscious and was resuscitated by the clinical team multiple times. His family was told to prepare themselves for the worst. Then, miraculously, he woke up.
The Aftermath
The time he spent in critical condition had caused him to lose a quarter of his body weight and his muscles to atrophy, so he needed help doing everything, even rolling over in bed. In addition, from being intubated so long, they discovered that his vocal cords were paralyzed and there was a major blockage of his airway requiring surgery to remove a large granuloma. His heart also required surgery to insert a permanent pacemaker to ensure that he didn’t go into cardiac arrest again. Once he was clinically stable to be discharged, Brian was transferred to inpatient rehab to continue his recovery.
Over a year later, Brian’s struggle is ongoing. He has been in and out of the hospital, he has contracted infections and needed a course of IV antibiotics at the hospital followed by home infusion of IV antibiotics. He needed pulmonary, occupational, and physical therapy.
He gets out of breath walking short distances, so he must rely on supplemental oxygen 100% of the time. He also requires a walker or a wheelchair to get around. “I used to be a very loud, boisterous individual and now I have to take a breath every few words and, if I am talking in a restaurant or somewhere with ambient noise, for example, it is very difficult for anyone to hear me. It’s a tremendous change of life,” he explained.
“It still takes its toll on me and my family,” he continued. “I am vaccinated and have received the booster, which offers some comfort, but obviously my body did not respond well to COVID-19 so we are constantly concerned about what might happen if I am ever exposed again.”
Finding Support after COVID-19
Aside from the physical toll it took on his body, Brian’s experience continues to be a psychological struggle. He found that the best way to deal was to talk with professionals and share his story with other people who have experienced the long-term devastation COVID-19 can create. This is how he came to join a one-of-a-kind support group hosted by Lisa Penziner, a registered nurse.
Lisa has a lot of experience leading support groups in many different facilities, such as Lynbrook Restorative Therapy and Glen Cove Rehabilitation on Long Island. Many of these groups specifically focused on lung disease patients through Better Breathers Club support groups. About a year into the pandemic, she realized that there was a pressing need for a post-COVID support group. “I noticed that many people that survived COVID-19 were experiencing odd symptoms months later that could not be explained. Some were physical (neuropathy, brain fog, fatigue, shortness of breath, hair loss) and some were psychiatric (PTSD, depression, anxiety, panic attacks), but at that time no one had answers as to how to address these problems. So, I decided to start the first post-COVID support group which included a discussion with myself and a psychologist colleague every two weeks on Zoom. The response was overwhelming.”
Lisa found that the need was a big one, and the meeting grew rapidly to include people all over the U.S and the Philippines. Brian was one of the first to join, and even calls himself the unofficial group “mascot.”
“We keep the meeting as light as possible, making sure everyone has an opportunity to discuss how they are feeling, and give advice to each other. We set measurable goals at each meeting so we can see how we did the next meeting. Some meetings we do relaxation and meditation to reduce anxiety.” said Lisa. “This is a place where the members can come be supported and voice their feelings of frustration or sadness.”
And that is exactly what it has done for Brian and what he hopes he is able to do for others by being part of the group. “It’s been terrific to talk to people and see their progress. There has been a good amount of turnover, which is great because we are able to let people know that what they are going through is real and they can work through it. It makes me feel great to help others, it gives me some self-worth, at a time when I often feel so helpless. The biggest thing is to give people information and hope, so they know they are not alone.”
Blog last updated: October 27, 2025