What Is Particle Pollution?
Particle pollution, also called “particulate matter” or “soot,” refers to a mix of tiny solid and liquid particles that are in the air we breathe. Ever look at dirty tailpipe exhaust or notice a haze in the air from wildfire smoke? A big part of what you see is particle pollution. Many of the particles are so small as to be invisible, but when their levels are high, the air becomes hazy and thick and they become noticeable. Particulate matter is one of six widespread air pollutants for which there are national air quality standards to limit their levels in the outdoor air.
Size matters.
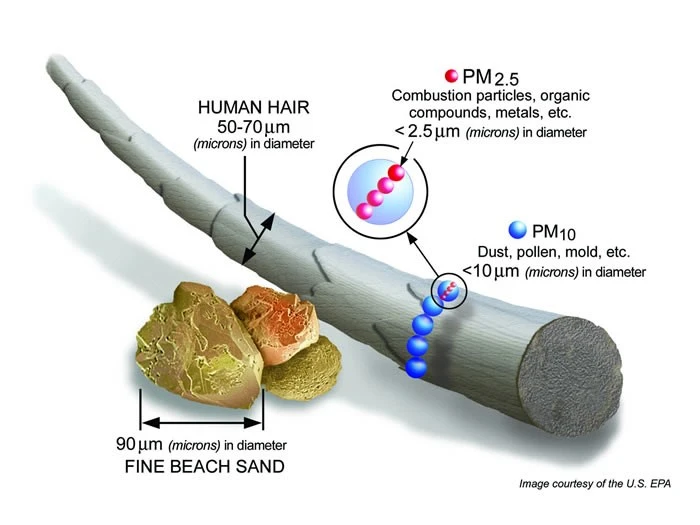
Particles themselves are of different sizes. Some are one-tenth the diameter of a strand of hair. Many are even tinier; some are so small they can only be seen with an electron microscope. Because of their size, you cannot see the individual particles. You can only see the haze that forms when millions of particles blur the spread of sunlight.
Particles are grouped according to size as coarse, fine and ultrafine. Coarse particles (shown as blue dots in the illustration) fall between 2.5 microns and 10 microns in diameter and are called PM10-2.5. Fine particles (shown as pink dots in the illustration) are 2.5 microns in diameter or smaller and are called PM2.5. Ultrafine particles (not shown) are smaller than 0.1 micron in diameter and are small enough to pass through the lung tissue into the blood stream, circulating like the oxygen molecules themselves. No matter what the size, particles can harm your health.
The differences in size make a big difference in how particles affect us. Our natural defenses help us to cough or sneeze some coarse particles out of our bodies. However, those defenses do not keep out smaller fine or ultrafine particles. These particles get trapped in the lungs, while the smallest are so minute that they can pass through the lungs into the bloodstream, just like the essential oxygen molecules we need to survive.
Particles are formed in different ways.
Some particles are liquid while some are solids suspended in liquids. As EPA put it, particles are really “a mixture of mixtures.”
Particle pollution forms through two separate processes—mechanical and chemical. Mechanical processes break down bigger particles into smaller bits with the material remaining essentially the same, only becoming smaller in size. Dust storms, construction and demolition, mining operations, and agriculture are among the activities that produce such particles. Road wear of tires, brake pads and other vehicle components can also create particles.
Chemical processes in the atmosphere create most of the fine and ultrafine particles in the air. Particle pollutants such as elemental black carbon (soot), volatile organic carbon compounds, heavy metals, and ammonia are released through chemical reactions such as burning fuels. Human activities and natural sources also emit gases that react in the air with other gases to form particles, such as when nitrogen dioxide and sulfur dioxide pollutants react with oxygen and water vapor in the air to form nitrate and sulfate particles.
What Are the Sources of Particle Pollution?
Combustion of carbon-based fuels generates most of the fine particles in our atmosphere. Burning wood in residential fireplaces and wood stoves as well as wildfires, agricultural fires and prescribed fires are some of the largest sources. Wildfires are growing, particularly in the western U.S. because of climate change. Burning fossil fuels in factories, power plants, diesel- and gasoline-powered motor vehicles (cars and trucks) and equipment emits a large part of the raw materials for fine particles.
What Are the Health Effects of Particle Pollution?
There is no safe threshold to breathe in fine particles. A recent review of all available scientific evidence to date clearly shows that particle pollution is associated with increased mortality from all causes, cardiovascular disease, respiratory disease and lung cancer.
Who Is at Risk?
While everyone is at risk from health impacts of outdoor particle pollution, those that live near the emission sources are at higher risk. Other vulnerable subpopulations at higher risk from particle pollution exposure include:
- Individuals who are pregnant;
- Infants, children and teens;
- Older adults (>65 years of age);
- People with lung disease, such as asthma and chronic obstructive pulmonary disease (COPD);
- People with cardiovascular disease;
- People who are obese or have diabetes;
- Current or former smokers;
- People with lung cancer;
- People with low socioeconomic status; and
- People of color.
What Can We Do about It?
The good news is that for much of the nation, the air generally has much lower levels of particulate matter now than in previous decades. Under the federal Clean Air Act, more protective standards nationwide have helped drive down the emissions that contribute to particulate matter. Power plants, industrial sites, vehicles and more are cleaner than they used to be, which has driven nationwide improvement in air quality. However, far too many people still live with unhealthy levels of particle pollution, and the emerging evidence continually shows that fine particles are more dangerous than previously understood. What’s more, climate change is driving increases in dangerous levels of particles from wildfire smoke.
Individuals can take steps to protect themselves on days with unhealthy levels of particle pollution, and policymakers at all levels of government can continue to require cleanup.
Page last updated: May 27, 2025