by Editorial Staff | July 16, 2018
- Impact
- Asthma
Jill Heins-Nesvold, MS, is National Director of Lung Health at the American Lung Association. Jill leads a team that works with clinics and hospitals nationwide to ensure professionals have the knowledge, skills and systems to provide the highest quality, guidelines-based asthma and COPD care.
Since 2010, I've had the immense pleasure in leading and working with members of the American Lung Association Lung Health Promotion team across the country to implement our Enhancing Care for Children with Asthma program. To date, our teams have worked with over 300 primary care clinics in 10 states to implement a 10-step quality improvement program to help support asthma management and care for children.
There are over 6 million children in the United States living with asthma, and through proper asthma management, children can live healthy and active lives like their peers. But, unfortunately, asthma is one of the main illness-related reasons that students miss school, accounting for 13.8 million lost school days each year. In this way, proper asthma management is directly related to academic performance, as well as costly medical expenses.
But the American Lung Association’s asthma educators are working to reverse that trend by providing direct support to the community clinics that are the first line of defense for children living with asthma. With one-on-one attention, our staff was able to provide extensive training for providers and other clinic staff on asthma diagnosis, medications, asthma management plans, ongoing asthma management and patient education. Equipment, patient education materials and technical assistance were also provided, giving healthcare providers the information, training and tools needed to help—families manage asthma symptoms.
This type of program looks different for the varying needs of each clinic. One particular clinic stands out in my mind, because when we first started working with staff, the number of patients with asthma were not known. Starting from square one, we had to ensure that clinic providers and nursing staff were trained on asthma diagnosis and management. We then helped them form an asthma registry, and medical records were updated with the diagnosis and severity of the patients' asthma.
Once patients were identified, an asthma self-assessment form was used to capture the frequency and types of symptoms that the patient had experienced over the past month, indicating their level of asthma control. After the initial assessment, providers ensured that asthma visits included:
- A review of asthma symptoms and any recent changes
- A lung function test (spirometry)
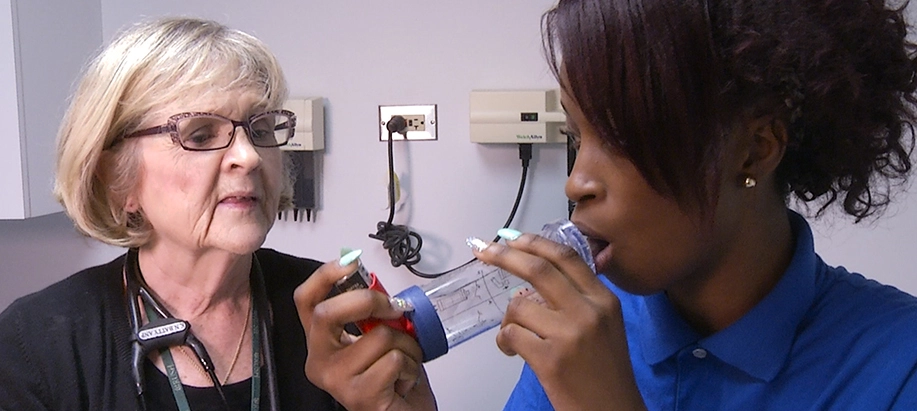
- Information on and the reassessment of long term controller and quick relief medication, how to self-administer, proper technique with a valved holding chamber and when to take
- Creation and review of an Asthma Action Plan
We were also able to connect all patients with an asthma educator to ensure that patients understood how to use an Asthma Action Plan and adjust it as necessary based on their symptoms. Nurses can also make referrals for patients interested in home-based environmental improvements for asthma and quit smoking support for adults in the home.
With funding from Health Care Service Corporation's Healthy Kids, Healthy Families Initiative, we were able to assess our work with 65 community health centers across four states. The work that was performed over that three-year project is being published in the Journal of Asthma, highlighting more than a 50 percent reduction in asthma-related emergency department visits and hospitalizations. The program dramatically improved the health of patients while also showing a significant savings for families and the healthcare system.
Programs like this truly show that with technical assistance, training, and time, we can make a difference in the lives of families affected by chronic lung disease. All children deserve to live healthy and active lives and I'm proud to be part of the team that helps them get there.
Blog last updated: October 15, 2025