How Acute Chest Syndrome Affects Your Body
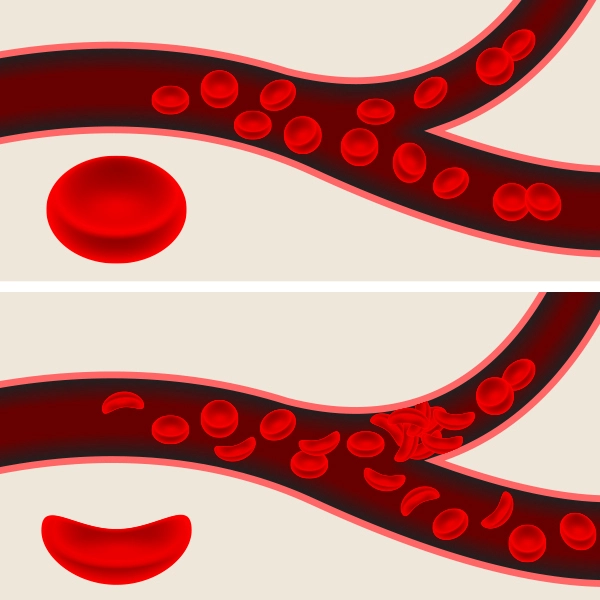
Hemoglobin is the protein in red blood cells that carries oxygen in your body. A person with sickle cell anemia makes a different type of hemoglobin called sickle hemoglobin. While normal red blood cells are shaped round, flexible and smooth, red blood cells that contain sickle hemoglobin develop an irregular shape like a crescent or banana.
Acute chest syndrome happens when these sickle cells block the small blood vessels in the lungs. This blockage reduces blood flow and the amount of oxygen that travels out to nourish the body. The longer the small blood vessels are blocked, the more damage can be done to other organs of your body.
Who Is at Risk?
There is no single cause of ACS, however certain conditions can trigger it. ACS can be brought on suddenly when the body is under stress from illness or dehydration.
- Other Medical Conditions: Pulmonary embolism (blood clots from other parts of the body travelling to the lungs), pulmonary fat embolism (bone marrow tissue travelling from the bones to the lungs), pulmonary artery thrombosis (blood clots forming in the lungs), infections like pneumonia, and asthma.
- Coronavirus disease 2019 (COVID-19) has been reported as a cause of ACS
- Vaso-occlusive crisis (VOC): Vaso-occlusive crisis (VOC) which is a common complication of SCD, presents with excruciating pain, usually of sudden onset, although it may be a gradual onset. The pain is often concentrated to the extremities like your arms and legs, chest or back. ACS may be a complication of VOC.
- Low oxygen levels: Low oxygen in the lungs and blood leads to the formation of sickle cells.
- Low Fetal Hemoglobin (HbF): Fetal hemoglobin or HbF is the main form of Hemoglobin in the fetus. HbF continues after birth and being in red blood cells protects against sickling. Low levels of HbF can increase the risk of ACS.
- Genotype: Sickle Hemoglobin is the product of the sickle gene S. Genes exist in pairs and individuals with SS have the most serious form of SCD. S may be present with another variation of the hemoglobin gene such as C which causes a less severe form of the disease.
- Age: ACS can occur at any age. In children with SCD peak onset of ACS occurs ages 2 to 4 years old.
- Infection: ACS in children is often triggered by infection
- Recent trauma or surgery: Due to pain and medications post-surgery, you may experience shallow breathing and low oxygen levels resulting in sickling in the lungs that cause ACS.
- Smoking or secondhand smoke exposure: Smoking or exposure to secondhand smoke is associated with a higher risk of ACS and more severe episodes in children.
Page last updated: October 23, 2024