Shortness of breath, cough, wheezing—these are just a few of the common symptoms of asthma that currently affects more than 25 million people living in America. Asthma is generally treated with a combination of quick-relief medicines, such as a rescue inhaler, as well as long-term maintenance medicines to keep the airways open (bronchodilation) and reduce inflammation in the lungs.
However, some people may not respond well to these medicines, and that is referred to as poorly controlled asthma, defined by the experience of daily symptoms, waking up at night from symptoms, or having more frequent flareups.
A recent study published by the American Lung Association Airways Clinical Research Centers (ACRC) in the Journal of Respiratory Medicine examined how a clinical test called the Bronchodilator Response is related to treatment outcomes in people with poorly controlled asthma.
Clinical Testing for Asthma
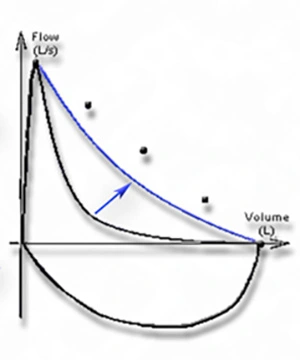
One of the most basic tests of lung function and health is called spirometry. In this test, patients take a full breath and blow as much air out of their lungs, as hard as they can, for as long as they can, followed by taking in a full breath. This is done at least three times to be as accurate as possible.
Spirometry can tell us a lot about lung function, but the most important measurements are the FEV1, or the Forced Expired Volume in 1 second, and the FVC, or the Forced Vital Capacity—both are recorded in liters of air. These metrics are then compared to numbers that are considered “clinically normal,” based on a person’s age, height, and sex. Any obstruction in the airway could reduce the FEV1, FVC, or both—that is one of the first clues that healthcare providers will use to determine that someone may have an obstructive lung disease such as asthma.
One clinical aspect that is used to diagnose asthma is its reversibility. In other words, if the spirometry in a person improves after given a quick relief/rescue bronchodilator, a medicine that helps relax the smooth muscles to open the airways. In the bronchodilator response (BDR) test, spirometry is performed at baseline (without medication), and then repeated 15 minutes after a dose of a bronchodilator. The change in FEV1 and FVC is considered the “response” to the quick-relief medicine. This means the amount of improvement in airflow based on the muscles relaxing. In the clinic, there are four definitions that would be considered a “positive” BDR, and those definitions range in how much the FEV1 or FVC change after being given the inhaler, such as by a percentage increase, a volume, or changes from the predicted values.
Research Challenging the Norm
In the study conducted by David Kaminsky, MD and other ACRC colleagues, the main aim was to determine if there was any link or relationship between the four different definitions of BDR and asthma control, along with the burden of asthma symptoms in a large population of individuals with poorly controlled asthma.
The study included over 900 participants and showed that 31-42% of participants met at least one of the four definitions of BDR. Also, the study found that BDR was more common in men, Black individuals, non-smokers, and non-obese participants. Among those with poorly controlled asthma, 35% exhibited a positive BDR, compared to 25% positive BDR among those with well-controlled asthma.
However, after adjusting for various factors, none of the four BDR definitions were associated with reported asthma control or symptoms. In other words, a positive BDR test was not necessarily related to the symptoms or asthma control.
Impacts of ACRC Research
This study is important because it questions the continued use of BDR by healthcare providers to assess how well a person’s asthma is being controlled. These findings will lead to further research and evaluation of new tools to improve the tracking and treatment of asthma. These tools, tests and scores could more accurately reflect the current disease state of a patient. The demographic findings also highlight that people with poorly controlled asthma need a customized treatment approach.
Research like this and other studies performed by the ACRC are critical to advancing our knowledge of lung disease and treatment, especially in long-established practices that may no longer be useful.
To learn more about the American Lung Association Airways Clinical Research Centers, visit lung.org/acrc. To learn more about asthma, visit Lung.org/asthma.
Blog last updated: October 23, 2025