It's no secret that quitting smoking significantly reduces the risk for a wide range of diseases and early death. Yet, tobacco use remains the leading cause of preventable death and disease in the U.S., and as of 2023, 10.8% of adults smoked cigarettes. While smoking rates in the U.S. reached their lowest ever recorded rates this decade, disparities persist. The 2024 Surgeon General’s report on “Eliminating Tobacco-Related Disease and Death: Addressing Disparities” found the burden of tobacco use remains higher in some communities, with disparities observed by geography, occupation, sexual orientation, gender identity, level of education, level of income, race and ethnicity, behavioral health status and disability status.13
These continued disparities highlight the uneven progress to curb tobacco industry marketing and enact policies proven to reduce tobacco use across the U.S. Here are 11 communities that are disproportionately affected by cigarette smoking and tobacco use, in no particular order:
1. Rural Communities
Adults who live in rural communities smoke at a rate of 15.4% compared to 10.1% among adults that live in urban areas. They are also more likely to smoke more heavily, smoking 15 or more cigarettes per day, compared to those who smoke and live in urban areas.1 Kids in rural areas are also more likely to start smoking at a much younger age and smoke daily, making addiction more severe and smoking harder to quit. Rural communities have more secondhand smoke exposure, youth isolation and the tobacco industry marketing their products to rural populations.2
2. Geographic Disparities
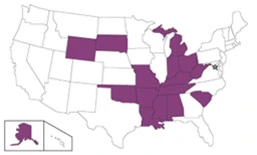
Adults who live in Midwestern and Southern states are more likely to smoke cigarettes than those in Northeastern and Western states.13 This largely coincides with the increased average smoking rate in the “Tobacco Nation” states (Alabama, Arkansas, Indiana, Kentucky, Louisiana, Michigan, Mississippi, Missouri, Ohio, Oklahoma, Tennessee and West Virginia)3 at over 40% higher than in other states.3 The Surgeon General’s report in 2024 noted several other states with similarly high smoking rates.13 For decades, tobacco industry lobbying has blocked tobacco control policies in Tobacco Nation states; however, over recent years, there has been some progress on implementing proven policies, including smokefree laws in these states and localities. Much more work remains.
3. Individuals with Blue Collar or Construction Jobs
Individuals with blue collar and construction jobs experience higher rates of smoking. Those who work in construction experience a 20.2% smoking rate. This is five times higher than the rate of smoking for jobs who experience the lowest rates of smoking. There are numerous reasons for this, including a lack of smokefree workplaces, less access to healthcare, including cessation treatment and lower wages.13
4. Military Veterans
Almost one in four military veterans use tobacco products, with close to 20% using combustible tobacco products like cigarettes and cigars, significantly higher than U.S. adults overall.4 Sadly, the military has a long history with tobacco use, including cigarettes previously being included with rations. Many veterans report beginning tobacco use in the military or reinforcing their tobacco use during their time in service.
5. Lesbian/Gay/Bisexual/Transgender Adults (LGBT)
Almost one in seven LGB* adults smoke cigarettes compared with about one in nine heterosexual adults.1 Even greater disparities are seen in e-cigarette use, with LGB adults nearly three times as likely to use e-cigarettes.1While nationwide data on tobacco use by gender identity has previously been limited, some evidence indicates that individuals who identify as transgender experience higher rates of tobacco use than those who do not identify as transgender or who identify as cisgender.13
LGBT individuals often face risk factors such as daily stress related to prejudice and stigma. The tobacco industry has a long history of aggressively targeting and marketing to the LGBTQ+ community, advertising in publications aimed at LGBTQ+ audiences and depicting tobacco use as an “accepted” part of LGBTQ+ life.5
* The statistic around this smoking rate does not include transgender individuals.
6. Adults Without a High School Degree
Adults with lower levels of educational attainment smoke at higher rates than the general population. Adults who did not graduate high school smoke at a rate of 18.3%, while adults with a high school degree smoke at a rate of 14.7%, and adults with an undergraduate degree smoke at a rate of 4.4%.1
7. Individuals with Lower Income
Individuals with incomes below the poverty threshold have a smoking rate of 19.5%.1 People living in poverty smoke cigarettes more heavily and smoke for nearly twice as many years as people with a family income three times higher.6 Lower-income individuals are also more likely to live in public housing, where smoking rates among adults are more than twice the national rate.7 Tobacco companies often target advertising campaigns toward low-income communities8 and a higher density of tobacco retailers can often be found in low-income neighborhoods.9
8. Individuals Without Health Insurance
Uninsured individuals in the U.S. smoke at a rate of 16.8%, double the rate of adults with private insurance, whose smoking rate is 8.4%.1 Research shows that gaining insurance coverage increases the odds of quitting smoking, due to more primary care visits, follow-up smoking assessments and smoking cessation medication ordered.10 The uninsured population includes approximately 1.4 million people in the ten states that have not expanded Medicaid that would be eligible for coverage, if their state expanded.11
9. Indigenous Communities
Indigenous peoples (American Indians/Alaska Natives) smoke commercial tobacco cigarettes at a rate of 15.0% and have the highest prevalence of cigarette smoking among all racial/ethnic groups in the U.S.1
It is important to distinguish between commercial tobacco use and tobacco use in traditional ceremonies as some members of Indigenous communities use tobacco for ceremonial, religious or medicinal purposes.
10. Individuals Living with Certain Behavioral Health Conditions
Individuals in the U.S. ever diagnosed with anxiety or depression smoke at a rate of 15.6%, compared to 9.3% among those never diagnosed.1 Even more alarming is that people with mental health conditions make up 25% of the population, but account for 39% of all cigarettes smoked.1 Nicotine’s mood-altering effects can also mask the symptoms of mental illness, putting people with mental health conditions at higher risk for nicotine addiction and cigarette use.12
In 2019, individuals who reported having an alcohol or illicit drug use disorder in the last year smoked at a rate of 37.8%.13 This is over three times the national smoking rate.
11. Individuals with a Disability
Individuals with a disability smoke at a rate of 16.9%, compared to those without disabilities who smoke at a rate of 10.2%.1 Individuals with disabilities can experience higher levels of stress, anxiety or other mental health conditions than their counterparts, which may contribute to a higher rate of smoking.
How Do We Keep Those at Greatest Risk from Being Left Behind?
All individuals deserve the chance to live a full and healthy life. Yet smoking rates are higher in certain parts of the country and among certain communities in the U.S. Complicating this crisis, the factors listed above tend to combine and compound the risk. For example, low-income adults are more likely to be uninsured.
Tobacco prevention and cessation efforts must focus on the policies called for in our “State of Tobacco Control” report, and ensure resources are directed toward communities most impacted by tobacco use and exposure to secondhand smoke.
Page last updated: February 5, 2026




.jpg?format=webp)


